3.1. Air
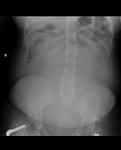
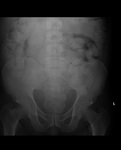
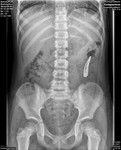
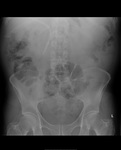
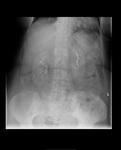
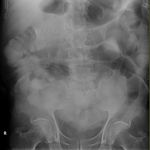
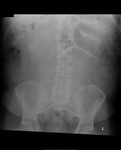
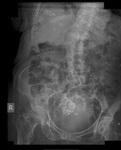
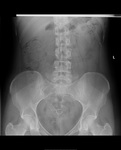
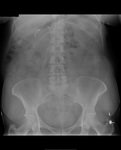
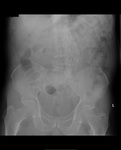
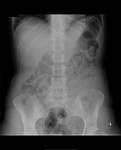
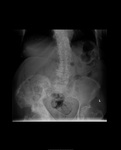
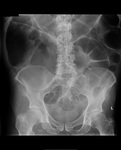
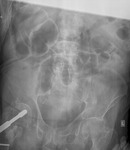
Air on an abdominal radiograph should only be seen within the bowel lumen. Air outside the bowel lumen is called pneumoperitoneum (figure 2). It is usually pathological, due to perforation of a hollow viscus, however may also be iatrogenic, such as in the early post-operative period. Free extraluminal gas can be identified on an abdominal radiograph through the following signs:
- Rigler’s sign: Normally only a single wall of bowel is visible on the abdominal radiograph (the inner wall of the bowel due to gas within the lumen opposing the bowel wall). However, in the case of pneumoperitoneum, gas is present on both sides of the bowel wall, hence both sides of the wall will be visible (figure 3).
- Air seen to lie along the inferior edge of the liver or outline the falciform ligament (figure 4).
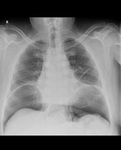
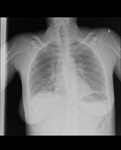
An erect chest radiograph is more sensitive at demonstrating pneumoperitoneum; as little as 1ml of free intraperitoneal air can be detected as free air under the diaphragm. Therefore, when pneumoperitoneum is suspected, an erect chest radiograph should be taken in conjunction with the abdominal radiograph. Air under the diaphragm is demonstrated by a well demarcated diaphragm due to air density on both sides (figures 5 and 6).
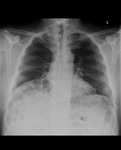
Chilaiditi’s phenomenon is bowel interposed between the liver and the right hemidiaphragm which may mimic free air on a chest radiograph and should not be confused with pneumoperitoneum (figure 7).
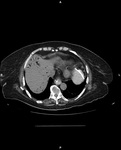
More uncommonly, air may be seen within the liver as pneumobilia or portal venous gas. Pneumobilia is air in the biliary tree due to an abnormal communication between the bowel and the biliary tree. This may be caused following sphincterotomy at endoscopic retrograde cholangiopancreatogram (ERCP) or due to a cholecysto-enteric fistula. Portal venous gas (figures 8 and 9) may be seen in bowel ischaemia or necrosis. The two can be differentiation according to the distribution of the air, with pnuemobilia being central, while portal venous gas being peripheral. This is however beyond the scope of an abdominal radiograph, and a CT should be advised.
3.2. Bowel
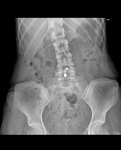
Small and large bowel can usually be differentiated by their location on the abdominal radiograph, with small bowel being central and large bowel being peripheral. Additionally, while small bowel demonstrates valvulae conniventaes which cross the full width of the bowel, the large bowel consists of haustral folds separated by pilicae semilunares, which are thicker and are not seen to completely traverse the bowel (table 1).
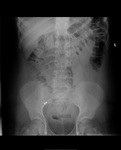
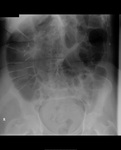
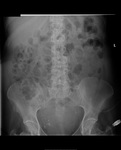
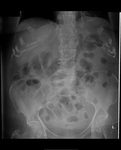
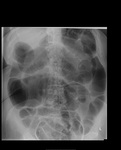
In small bowel obstruction (figure 10) the small bowel is typically dilated more than 3cm, with prominence of the valvulae conniventes. The more distal the obstruction, the greater the number of loops visible on the radiograph.
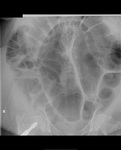
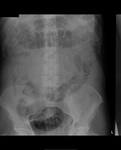
Large bowel obstruction (figure 11) can be divided into open or closed loop, depending on ileo-caecal valve competency. There is a higher risk of perforation in closed loop obstruction.
Volvulus (figure 12) is an uncommon cause of acute obstruction. It results when the colon twists on its mesentery causing a closed loop obstruction. Sigmoid volvulus is the most common and has the characteristic ‘coffee bean’ sign due to apposed medial walls of the affected loops of bowel.
Another pathology affecting the large bowel which may be picked up on an abdominal radiograph is colitis. The most common causes of colitis are infections, inflammatory bowel disease, ischaemia and radiotherapy. Signs that may be noted include the following:
-
Thumb printing: non-specific sign caused by mucosal oedema.
-
Toxic megacolon: dilated transverse colon or progressive distension on serial radiographs without obstruction.
-
Lead-pipe colon: due to chronic colitis causing atrophy and scarring of mucosa with resultant absence of haustrae.
3.3. Densities
Calcifications:
-
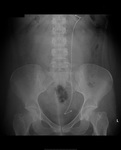
Renal tract calculi: Although an abdominal radiograph is not the imaging of choice when assessing for calculi of the renal tract, radio-opaque calculi may be an incidental finding (figure 13).
-
Phleboliths: These are small venous mural calcifications. They are common and the incidence increases with age. They have no clinical significance, however it is important to note that they can be confused with renal calculi (figure 14).
-
Appendicoliths: Calcifications seen in the projection of the right iliac fossa may be consistent with appendicoliths.
-
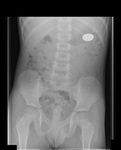
Gallstones: 10% of gallstones are visible on plain abdominal radiographs and may be an incidental finding (figure 15).
-
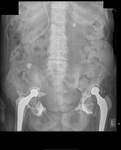
Vascular calcification due to atherosclerosis: This may be useful in the detection of aneurysms (figure 16). If an aneurysm is suspected, further imaging should be recommended.
-
Retroperitoneal calcification: Chronic pancreatitis (figure 17) may be seen as calcification following the anatomical position of pancreas and adrenal calcification may be seen following previous haemorrhage or TB.
-
Costochondral calcifications (figure 18)
- Calfication of masses and tumours, e.g. uterine fibroid (figure 19)
Bones:
-
The bones visualised on an abdominal radiograph include the lower ribs, lumbar spine, sacrum, pelvis, proximal femora
-
Abnormal bone findings may include:
-
-
Fractures (see figure 16)
-
Paget's disease (figure 20)
-
Bone lesions (sclerotic or lytic)
- Joint disorders: degenerative changes, osteitis condesans ilii (figure 21)
- It is important to note that bowel gas may give a false impression of lytic lesions
3.4. Organs and Soft Tissues
The organs and soft tissues which can be appreciated to a greater or lesser degree include the liver, spleen, kidneys, psoas muscles, bladder and the lung bases .Each separate organ, however, shows very limited detail, and the appropriate imaging modality should be selected on a case by case basis.
The liver and spleen are projected as a soft tissue density structures in the right and left upper quadrants respectively.
The gallbladder is rarely appreciated on an abdominal radiograph. Calcified gallstones (see figure 15) or cholecystectomy clips may sometimes be visualized (figure 22).
The psoas muscles are hip flexors, the borders of which may be obscured if there is an abdominal mass (figures 23 and 24). The kidneys may be visible at level T12-L3, the right kidney usually slightly lower due to the liver.
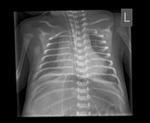
The lung bases should be visualized on a properly taken abdominal radiograph and must be taken into consideration when reporting. A basal pneumonia may be the cause of abdominal pain and lung metastases may be a known or an incidental finding.
3.5. External Objects and Artifacts
Devices which are external to the patient may be radio-opaque and hence visible on an abdominal radiograph. This may give useful clinical information, such as the position of tubes and stents, and therefore a good knowledge of anatomy and correct positioning is essential. Other devices may be irrelevant, however recognition of such items is still necessary to avoid misinterpretation.
External devices may be medical:
- Nasogastric or nasojejunal tubes (figure 25)
- Pig tail ureteric stents (figure 26)
- Colonic stents
- IVC filters (figure 27)
- Biliary stent (figure 28)
- Intra-uterine device (figure 29)
- Embolization coils (figure 30)
- Endovascular aortic repair (figure 31)
- Surgical clips
- Pessaries
They may be foreign bodies ingested accidentally or intentionally:
- Body packing (figure 32)
- Swallowed foreign objects (figures 33, 34 and 35)
They may be insignificant but present:
- Jewellery (naval piercings) (figure 36)
Knowing what imaging procedures the patient has undergone is necessary as residual contrast from previous scans may also be seen, interfering with the imaged structures (figure 37).